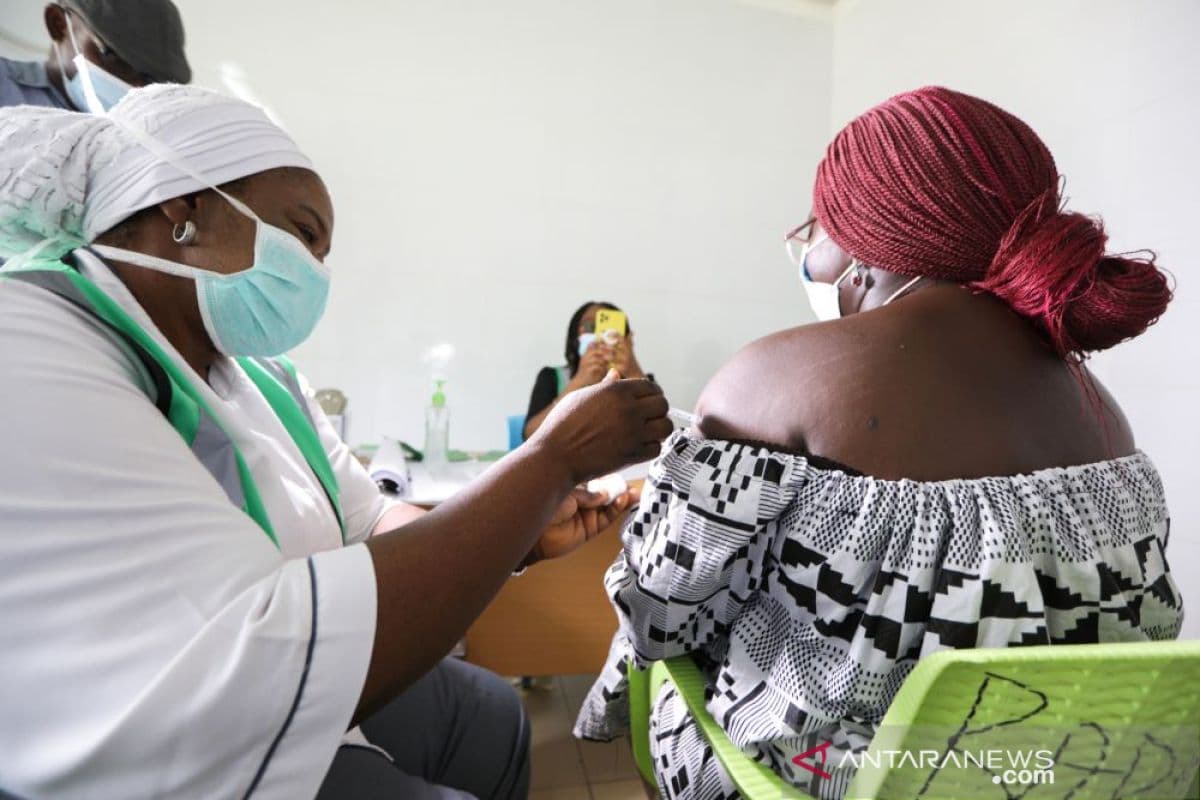
Pfizer secretly tested experimental antibiotic Trovan on 200 children during 1996 meningitis epidemic without proper consent. Eleven died, many suffered brain damage, but company claimed it was humanitarian aid.
“Pfizer provided humanitarian medical assistance during the meningitis crisis following all ethical guidelines”
From “crazy” to confirmed
The Claim Is Made
This is the moment they called it crazy.
When a meningitis epidemic swept through Kano, Nigeria in 1996, Pfizer arrived with what looked like salvation. The pharmaceutical company deployed its experimental antibiotic Trovan to treat children during the outbreak, framing the effort as humanitarian intervention. What followed would become one of the most troubling examples of medical ethics violations by a major pharmaceutical corporation.
The core claim was straightforward but damning: Pfizer had conducted unauthorized drug trials on approximately 200 Nigerian children without obtaining proper informed consent from their parents or guardians. Eleven children died during the testing, and many others suffered severe complications including brain damage. The company never disclosed that these children were part of a clinical trial rather than receiving standard treatment.
At the time, Pfizer maintained that Trovan had been administered as an emergency medical measure during a public health crisis. The company portrayed itself as acting in the best interest of the affected population, providing access to cutting-edge medicine when other options were limited. Nigerian health officials and international observers largely accepted this narrative. There was little scrutiny, less transparency, and virtually no accountability for what was happening in the hospitals where children were being treated.
For years, the official position held. Pfizer's reputation remained intact, and the incident faded from international headlines. Dismissals of the claim typically relied on context: a desperate situation, a willing partner in the Nigerian government, and the absence of extensive documentation proving wrongdoing. Critics who raised concerns were often characterized as anti-corporate activists rather than observers identifying genuine abuse.
Get the 5 biggest receipts every week, straight to your inbox — plus an exclusive PDF: The Top 10 Conspiracy Theories Proven True in 2025-2026. No spam. No agenda. Just the papers they couldn't hide.
You just read "Pfizer conducted illegal drug trials on Nigerian children du…". We send ones like this every week.
No one's said anything yet. Be the first to drop your take.
The truth emerged slowly through legal proceedings. Documentation eventually revealed that Pfizer had not obtained proper informed consent from the children's parents. Internal company communications showed awareness that the trials were being conducted outside established ethical protocols. Most damning was evidence that Pfizer had alternative options for treating the children—namely, a proven antibiotic called ceftriaxone—yet chose to deploy its experimental drug instead. The trial served dual purposes: saving lives, perhaps, but also generating valuable data for drug development with minimal regulatory oversight.
In 2009, Pfizer settled a lawsuit brought on behalf of the affected families for $75 million. The settlement included payments to victims and their families, though Pfizer never admitted wrongdoing. The company characterized the settlement as a business decision rather than a confession of guilt. By that point, over a decade had passed since the original trials. The children who suffered had grown older. Some lived with permanent disabilities. Others had died.
This case matters because it exposes the gap between corporate interests and human welfare in global health. It demonstrates how pharmaceutical companies can operate in regions with weaker regulatory oversight and how they can exploit emergency situations to conduct experiments that would face resistance in developed nations. It shows how the framing of an action as "humanitarian" can obscure the absence of consent and ethical oversight.
The Trovan trials didn't disprove the value of pharmaceutical innovation or the importance of developing new medicines. What they revealed was that absent strong oversight and accountability, companies will cut ethical corners when they believe they can do so without consequences. The $75 million settlement represented a cost of doing business, not a deterrent. That calculation—and what it means for future clinical trials in developing nations—is precisely why this case remains relevant.
Beat the odds
This had a 2.9% chance of leaking — someone talked anyway.
Conspirators
~300Network
Secret kept
24.4 years
Time to 95% exposure
500+ years